Psoriasis is a chronic skin condition in which a rapid buildup of skin cells causes red, raised, and cracked scaly patches, most often on the elbows, hands, feet, and knees. In the United States, over seven million people endure the physical pain, embarrassment, and reduced confidence that go hand-in-hand with this inflammatory condition.
Thanks to a greater understanding of the inflammatory pathways that cause psoriasis, treatments have improved tremendously over the past decade. Dr. Lauren Dickson, a Board Certified Dermatologist, contributes to peer-reviewed journals and lectures about the latest advances in psoriasis treatment. Presently, although there is no cure, Dr. Dickson and her partners at Dallas Dermatology Partners can prescribe a systemic, topical, or phototherapy treatment that can improve psoriasis symptoms and help restore your self-confidence.
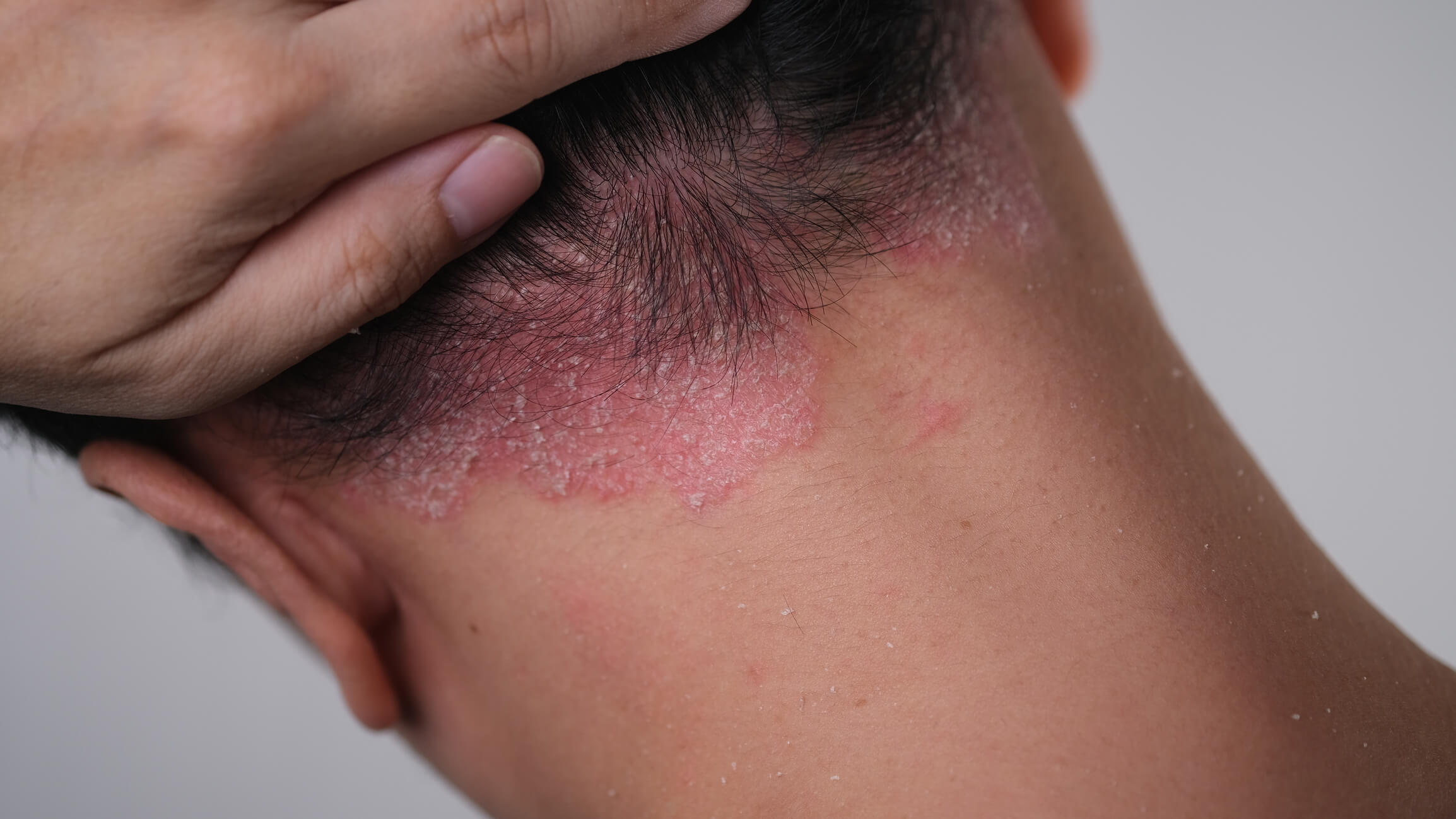
Types of Psoriasis
It is possible to develop more than one of the seven different types of psoriasis. Whether you have mild or severe symptoms, it's best to see a dermatologist before the condition worsens.
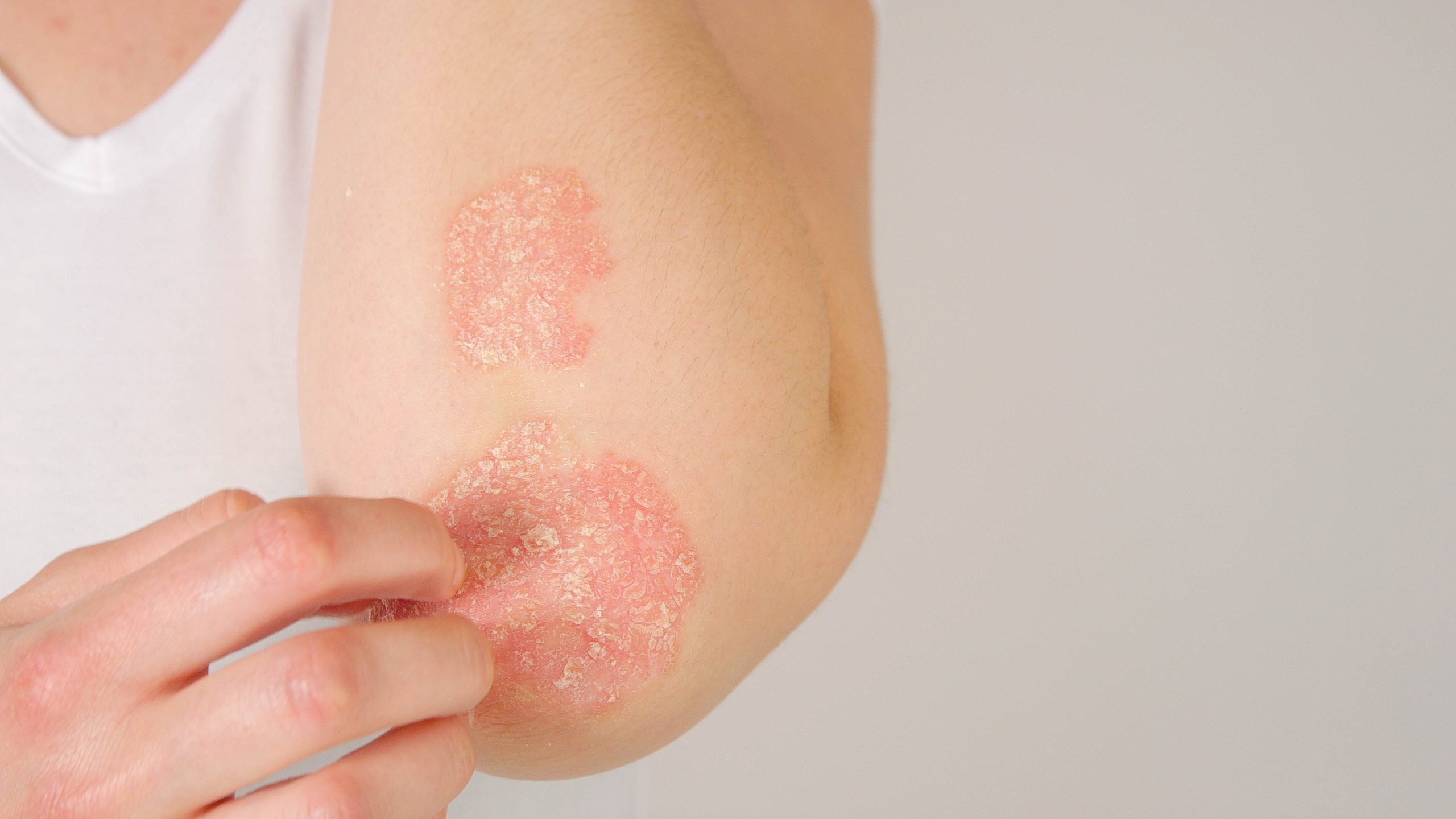
- Plaque Psoriasis – Plaque psoriasis affects about 80% of patients and can be found on the knees, scalp, elbows and back as raised red lesions covered in silvery-white scales.
- Guttate Psoriasis – This type often presents during childhood or early adulthood and is characterized by small red spots on the torso and limbs. Bacterial infections such as strep throat may be a trigger for it.
- Inverse Psoriasis – Inverse psoriasis causes bright-red lesions in the armpits, groin, under the breasts, or other skin folds. Sweat and friction often aggravate the lesions, causing additional pain and irritation.
- Pustular Psoriasis – Often triggered by medication, ultraviolet light, pregnancy, or infection, pustular psoriasis causes white, pus-filled blisters surrounded by red areas of skin.
- Erythrodermic Psoriasis – This is a rare form of psoriasis that causes generalized redness and scaling involving a large area of the body. The consequences can be serious if left untreated.
- Nail Psoriasis - Nail psoriasis results in thickened and yellow nails, sometimes with visible pitting.
- Psoriatic Arthritis – Slightly less than one-third of patients will have psoriatic arthritis. Symptoms include stiffness and pain in the joints that can be debilitating. Left untreated, it can result in permanent joint damage.
Psoriasis Treatments
Although psoriasis is a chronic disorder, it can be effectively managed with proper treatment that targets the inflammation. The goal is to clear up symptoms and interrupt the abnormal skin cell production cycle. There is no 'one-size-fits-all' modality for managing it. Treatment plans are tailored to the individual and depend on the type and the extent of the symptoms.
Treatments may include one or a combination of the following therapies:
- Topical Treatments – Topical ointments like vitamin D, corticosteroids, or topical retinoids target skin-cell growth, and inflammation to relieve mild or moderate symptoms.
- Phototherapy – Exposure to natural sunlight or narrowband Ultraviolet-B light (NBUVB) helps slow the production of skin cells, which improves the skin's overall appearance.
- Oral Medication – Vitamin A, apremilast, methotrexate, or cyclosporine can help calm symptoms in more severe cases.
- Biologics – Biologics are administered by injection or IV infusion and are effective at treating plaque psoriasis and psoriatic arthritis. They work by blocking specific parts of the immune system that cause plaque formation or joint damage. Biologics can be life-changing treatments for patients who do not respond to other modalities. The majority of biologics can be self-injected at home after training by your dermatologist.
A regular skincare routine of gentle cleansing and moisturizing can also go a long way towards reducing symptoms. Patients are also encouraged to avoid triggers like alcohol, stress, and smoking and keep the affected areas covered during sleep to reduce irritation.
What Causes Psoriasis?
Psoriasis is considered an immune-system disorder that has genetic and environmental components. It affects white blood cells, or "T cells" responsible for fending off viruses and other foreign bodies. In psoriasis patients, T cells attack healthy skin cells causing the over-production of new skin cells. As they accumulate, characteristic scaling and dry patches develop.
Symptoms usually manifest in cycles of remissions and flare-ups. Common psoriasis triggers include:
- Throat infections
- Injury to the skin
- Cold, dry weather
- Stress
- Smoking
- Heavy alcohol consumption
- Systemic steroid use
- Certain medications
Psoriasis Symptoms
Symptoms will depend on the type and amount of psoriasis you have, but usually include:
- Red or pink raised plaques covered with silver-colored scales
- Dry and crusting skin
- Cracked skin that can bleed easily
- Burning or itching skin
- Pain or soreness
- Thickened and discolored nails
Plaques can be limited to a few tiny areas or affect large areas of skin. Painful, itchy patches on the palms, groin, or soles of the feet can be especially bothersome, impacting the overall quality of life.
Our board-certified dermatologists understand that psoriasis is a complicated condition that has both physical and psychological components. Since it can have systemic inflammatory effects on the joints, cardiovascular system, and other organs, psoriasis requires continual monitoring and evaluation. Further, with age, your psoriasis treatment needs will likely change over time.
Psoriasis Dermatologist
Living with psoriasis can be a challenge, but with the right medical guidance and support from Dallas Dermatology Partners, it can be effectively managed and controlled. Our physicians and entire staff are dedicated to providing compassionate skincare for psoriasis patients in the Dallas/Fort Worth area.
If you're curious about a new psoriasis treatment or need a diagnostic evaluation, call today to schedule your Psoriasis appointment.
